
Blog by Joe Babaian
It’s about looking at the patient as a unique individual, that’s precision medicine, the future ~ @RasuShrestha
Less than 20% of US Hospitals have deployed precision medicine solutions. ~ @HIMSSAnalytics
I’ve been considering the inexorable forward momentum of the blurred combination of technology and healthcare. You feel it. Things are speeding up. With that forward velocity comes more than a few bumps and wrong turns, but like that feeling you get once you hit the Interstate or Autobahn, you know you are going to get there.
Quick reminder: What is Precision Medicine?
According to the National Institutes of Health (NIH), precision medicine is “an emerging approach for disease treatment and prevention that takes into account individual variability in genes, environment, and lifestyle for each person.” Personally, I prefer @RasuShrestha’s more succinct definition above.
 Photo credit: @RasuShrestha
Photo credit: @RasuShrestha
Recently, Tom Sullivan of Healthcare IT News talked to Dale Sanders, EVP at Health Catalyst. In the piece, AI, machine learning will shatter Moore’s Law in rapid-fire pace of innovation, Dale was very clear about what’s going on right now:
I’ve never in my career seen the acceleration of technology as fast as what we’ve witnessed in machine learning during the last two years.
Reviewing the journal article, The path from big data to precision medicine, we are reminded (in quite the understatement):
The volume and velocity of data generated presents problems when considering data processing, storage, and interpretation.
 First, we grasp the tremendous amount of data being generated, the need to filter, clean, parse, and then we seek to learn from the intricate and subtle connections therein. We find ourselves requiring the advancing toolsets of machine learning and artificial intelligence systems to realize the ultimate fruition of precision medicine’s promise. The ability of big data to be truly useful is within the grasp of humanity’s ingenuity and technology tools.
First, we grasp the tremendous amount of data being generated, the need to filter, clean, parse, and then we seek to learn from the intricate and subtle connections therein. We find ourselves requiring the advancing toolsets of machine learning and artificial intelligence systems to realize the ultimate fruition of precision medicine’s promise. The ability of big data to be truly useful is within the grasp of humanity’s ingenuity and technology tools.
Selected Applications
Cancer –
At the Englander Institute for Precision Medicine at Weill Cornell Medical College, director Dr. Mark Rubin explains:
Our goal is to use precision medicine to improve the way clinicians think about cancer therapies as opposed to selecting a therapy that may not be fitted to that patient’s cancer.
In their study, Personalized In Vitro and In Vivo Cancer Models to Guide Precision Medicine, Weill Cornell investigators found, “Combining genetic information from a patient’s tumor cells with three-dimensional cell cultures grown from these tumors and rapidly screening approved drugs can identify the best treatment approaches in patients for whom multiple therapies have failed.”
Precision medicine and oncology have been a natural fit as research continues to view cancer itself as often exceedingly personal in its expression for any given individual. Oncology, in many ways, has proven to be the proving grounds for precision medicine.
Pharma –
Within Personalized medicine: Time for one-person trials, Nicholas J. Schork explains:
Key to making precision medicine mainstream is the ongoing shift in the relationship between patients and physicians. A major advantage of the N-of-1 approach over classical trials is that patients are no longer guinea pigs, whose involvement in a study may help only future generations. In N-of-1 trials, the effectiveness of different treatments are vetted for the actual participants. Indeed, members of hundreds of patient-advocacy groups, for instance for rare genetic diseases, are eager to be involved in studies to test candidate drugs.
Thinking about the extended implications of personal treatment at the N-of-1 (much gratitude to @CancerGeek here), I can’t help but see how obvious it feels that this is the right way vs. the “one-size-fits-all” false efficiency of how we have done medicine for so long. Of course, this shift isn’t as simple as an “obvious” feeling and idea – the hard work of research and application continues. Here is an excellent example of this false efficiency – at least when it comes to pharma:
 Photo: Nature 520, 609–611; 2015
Photo: Nature 520, 609–611; 2015
Care Delivery –
At the Duke Center for Research on Personalized Health Care, they’ve turned to a model of precision care based on a clear underlying premise:
Disease develops dynamically as a consequence of inherited genetic susceptibilities and resistances, influenced by environmental factors. At the Duke Center for Research on Personalized Health Care, we reason that, with available and emerging tools, risk for disease can be quantified and prevention measures initiated before pathology develops — and that when it does, its mechanisms can be identified so that disease is treated with precision.
Take a look at what Duke has designed to flip care around to become proactive vs. reactive:

When discussing their vision for redesigning clinical care, Duke reminds us of a piece of history and why it is still significant. I know many of you out there have seen or heard of this report. I have linked to a PDF – take a look back over 100 years in order to see the future:
The 1910 Flexner Report shocked the medical establishment into incorporating scientific advances to transform how disease is defined, diagnosed, and treated. More than a century later and a decade since the genomic revolution, it’s again time to redesign clinical care to also enhance health and prevent disease.
What’s Next
I like Reenita Das’ recent article in Forbes, Drug Industry Bets Big On Precision Medicine: Five Trends Shaping Care Delivery, because she nails five major trends in care delivery – and it’s not just Pharma making the big bets.
- Unreasonable cost of trial-and-error medicine makes precision medicine imperative for targeted therapies
- Scientific and technological advances in the genomics field mean that cost and time are no longer a barrier for precision medicine
- The precision medicine focus goes beyond oncology: new companion diagnostic (CDx) and biomarkers for non-oncology therapeutic areas
- Precision medicine will harness healthcare big data to elevate preventive care for chronic disease management
- Precision medicine will boost the healthcare consumerism moment

Photo: Reenita Das
It’s The Data
If you have been around #hcldr for even a short time, you know we talk a lot about bringing care to where the patients are – physically, emotionally, and financially. This is a core concept that breaks down the wall with the small door labelled, “One size fits all.”
Part of bringing care to the people includes the inclusion of as many of them as possible in diverse data sets and cohort analysis. What a skew we’d have if we collect data only from people who are willing and able to come to the clinic during the hours we select! The solution? What was known as The Precision Medicine Initiative (PMI) Cohort is now called the All of Us Research Program – check it out. The goal? To collect biosamples from at least one million patients to fuel big data analytics and personalized [precision] medicine research.
The Duke Initiative for Science & Society Science Policy Tracking Program shares:
While a National Institutes of Health survey from 2016 indicated that patients are generally very interested in contributing genetic, clinical, and environmental data to one of the nation’s most ambitious research projects, collecting data from patients at scale is a significant logistical and technical challenge. The strategy [All of Us Research Program] may bring two key benefits: increasing the convenience factor for contributors and reaching patient populations that may be homebound due to illness, those who lack access to transportation, or individuals who maintain only infrequent contact with the healthcare system.
Perhaps this can be called, “Flip the research project?” I like it! Turning things around to meet the people – participants where they are.
While we are on data, this chart from The path from big data to precision medicine does a wonderful job outlining the types and characteristics of big data you encounter in precision medicine. It’s detailed, so please click for the larger size (and to save a copy).
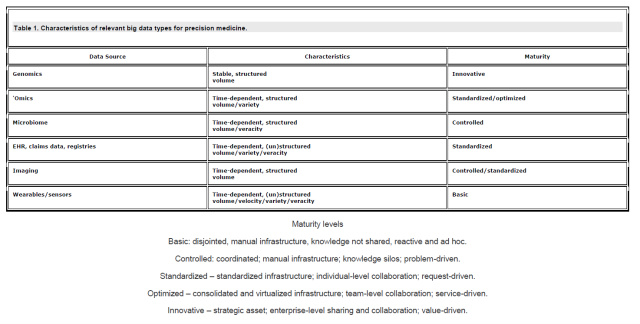 Chart: The path from big data to precision medicine
Chart: The path from big data to precision medicine
In addition, from the same publication, here’s a representation of all the data types/sources that are or will be collected for precision medicine and, by that measure, a great representation of the future of big data itself.
In the future, precision medicine will be enabled by individuals surrounded by a cloud of data. Layers of the cloud represent data varying between those directly affecting/quantifying the individual, and those quantifying the environment and indirectly affecting the individual, i.e. levels of the exposome.

Diagram: The path from big data to precision medicine
Let’s look at where we are today and where we want to be tomorrow. I readily acknowledge the amount of hype surrounding any new technological change; especially precision medicine/machine learning/AI. Precision medicine, facilitated by deep learning and artificial intelligence, is a behemoth of complexity, possibility, and reality. It’s perfect for both positive shifts and dead-ends.
What will you do now that you are armed with the information, the background, and the desire to accelerate straight down that Interstate? To a place where the oncologist no longer ever has to say, “We tried to successfully treat, but…” No. More. Buts. Let’s create the future beyond today, within reach.

Please join the #hcldr community of friends and peers as we work to make a difference, one idea and one action at a time. Join us on Tuesday, April 11, 2017 at 8:30pm Eastern (for your local time click here) as we discuss the following topics:
- T1: What do you see as the most significant promises of precision medicine? What will be impacted the most?
- T2: What challenges will stand in the way of advancing precision medicine/machine learning/AI?
- T3: What are the risks as healthcare is increasingly delivered based on AI analysis, custom for each patient (and fast)?
- T4: How will these changes impact future doctors, nurses, and clinics? Will hospitals change?
Resources for Further Study
“All of Us Research Program.” National Institutes of Health (NIH). Accessed April 11, 2017. https://www.nih.gov/research-training/allofus-research-program.
Bresnahan, Samantha. “The Isolated Island That Could Reveal New Medicines.” CNN, March 16, 2017. http://www.cnn.com/2017/03/16/health/iceland-genes-genealogy-alzheimers-exp/index.html.
“Changing Medicine with 3-D Bioprinting, Where Organs Can Be Synthesized by Technology.” Los Angeles Times, February 23, 2015. http://www.latimes.com/brandpublishing/localplus/ucsandiego/la-ss-ucsd2015-3dbioprinting-dto-story.html.
Das, Reenita. “Drug Industry Bets Big On Precision Medicine: Five Trends Shaping Care Delivery.” Forbes, March 8, 2017. http://www.forbes.com/sites/reenitadas/2017/03/08/drug-development-industry-bets-big-on-precision-medicine-5-top-trends-shaping-future-care-delivery/.
Dvorak, Katie. “Columbia’s David Goldstein: Precision Medicine Will Change Disease Treatment Paradigm | FierceHealthcare,” September 30, 2016. /it/columbia-s-david-goldstein-precision-medicine-will-change-disease-treatment-paradigm.
“FAQ About Pharmacogenomics.” National Human Genome Research Institute (NHGRI), May 2, 2016. https://www.genome.gov/27530645/FAQ-About-Pharmacogenomics.
Flexner, Abraham. “Carnegie Foundation | eLibrary | Medical Education in the United States and Canada Bulletin Number Four (The Flexner Report).” The Carnegie Foundation for the Advancement of Teaching, 1910. http://archive.carnegiefoundation.org/publications/medical-education-united-states-and-canada-bulletin-number-four-flexner-report-0.
Gibson, Mara L, Kenneth C Hohmeier, and Cindy T Smith. “Pharmacogenomics Testing in a Community Pharmacy: Patient Perceptions and Willingness-to-Pay.” Pharmacogenomics 18, no. 3 (January 23, 2017): 227–33. doi:10.2217/pgs-2016-0161.
HealthITAnalytics. “Mayo Gets $142M to Create Precision Medicine Initiative Biobank.” HealthITAnalytics, May 31, 2016. http://healthitanalytics.com/news/mayo-gets-142m-to-create-precision-medicine-initiative-biobank.
———. “NIH Renames Precision Medicine Cohort, Urges Patient Engagement.” HealthITAnalytics, February 7, 2017. http://healthitanalytics.com/news/nih-renames-precision-medicine-cohort-urges-patient-engagement.
“HIMSS Analytics.” Accessed April 11, 2017. http://www.himssanalytics.org/presentations/precision-medicine?utm_source=twitter&utm_medium=social&utm_campaign=2017precision.
Huang, Bevan E., Widya Mulyasasmita, and Gunaretnam Rajagopal. “The Path from Big Data to Precision Medicine.” Expert Review of Precision Medicine and Drug Development 1, no. 2 (March 3, 2016): 129–43. doi:10.1080/23808993.2016.1157686.
Huser, Vojtech, Murat Sincan, and James J Cimino. “Developing Genomic Knowledge Bases and Databases to Support Clinical Management: Current Perspectives.” Pharmacogenomics and Personalized Medicine 7 (September 9, 2014): 275–83. doi:10.2147/PGPM.S49904.
“NIH to Bring Precision Medicine Data Collection to Patient Homes.” SciPol, April 7, 2017. http://scipol.duke.edu/content/nih-bring-precision-medicine-data-collection-patient-homes.
Olson, Maynard V. “A Behind-the-Scenes Story of Precision Medicine*.” Genomics, Proteomics & Bioinformatics 15, no. 1 (February 2017): 3–10. doi:10.1016/j.gpb.2017.01.002.
Pauli, Chantal, Benjamin D. Hopkins, Davide Prandi, Reid Shaw, Tarcisio Fedrizzi, Andrea Sboner, Verena Sailer, et al. “Personalized In Vitro and In Vivo Cancer Models to Guide Precision Medicine.” Cancer Discovery, March 22, 2017. doi:10.1158/2159-8290.CD-16-1154.
Ralph Snyderman; Caroline Meade; Connor Drake, MPA. “To Adopt Personalized Health / Precision Medicine, Redesign Clinical Care.” NEJM Catalyst, February 5, 2017. http://catalyst.nejm.org/adopt-precision-medicine-personalized-health/.
Reference, Genetics Home. “What Is the Difference between Precision Medicine and Personalized Medicine? What about Pharmacogenomics?” Genetics Home Reference. Accessed April 11, 2017. https://ghr.nlm.nih.gov/primer/precisionmedicine/precisionvspersonalized.
Robinson, Peter N. “Deep Phenotyping for Precision Medicine.” Human Mutation 33, no. 5 (May 2012): 777–80. doi:10.1002/humu.22080.
Schork, Nicholas J. “Personalized Medicine: Time for One-Person Trials.” Nature News 520, no. 7549 (April 30, 2015): 609. doi:10.1038/520609a.
Shrestha MD MBA, Rasu. “3 Key ONC #PrecisionMedicine Initiatives: Sync for Science (S4S) S4S Privacy & Security Sync for Genes #HIMSS17 https://Www.nih.gov/Allofus-Research-Program …pic.twitter.com/lisrQpY0um.” Microblog, February 19, 2017. https://twitter.com/RasuShrestha/status/833354986159497216.
———. “Less than 20% of US Hospitals Have Deployed Precision Medicine Solutions. #PrecisionHIT. http://Ow.ly/jsTZ100CIcb Pic.twitter.com/lBYO3AQ5xI.” Microblog, March 25, 2017. https://twitter.com/RasuShrestha/status/845731948958011392.
Sullivan, Tom. “AI, Machine Learning Will Shatter Moore’s Law in Rapid-Fire Pace of Innovation.” Healthcare IT News, April 7, 2017. http://www.healthcareitnews.com/news/ai-machine-learning-will-shatter-moores-law-rapid-fire-pace-innovation.
“Three-Pronged Approach Key to Precision Medicine | Caryl and Israel Englander Institute for Precision Medicine,” March 22, 2017. http://ipm.weill.cornell.edu/news/three-pronged-approach-key-precision-medicine.
Timmerman, Luke. “What’s in a Name? A Lot, When It Comes to ‘Precision Medicine.’” Xconomy, February 4, 2013. http://www.xconomy.com/national/2013/02/04/whats-in-a-name-a-lot-when-it-comes-to-precision-medicine/.
Wykes, Sara. “Design Thinking as a Way to Improve Patient Experience.” News Center, June 3, 2016. http://med.stanford.edu/news/all-news/2016/06/design-thinking-as-a-way-to-improve-patient-experience.html.
Photo Credit: http://imgur.com/a/hjtIz